Associated diseases
- Title: Associated diseases
- Subtitle: Melisa
- Intro text editor:
People with metal hypersensitivity may have numerous symptoms associated with an overactive immune system, including chronic fatigue, joint and muscle pain, cognitive impairment, depression, headaches, fibromyalgia and skin rashes.
The article A comprehensive summary of disease variants implicated in metal allergy lists hundreds of publications describing metal-specific allergy responses, identifying over 50 unique manifestations. According to the authors, metals constitute one of the major classes of allergens responsible for a disproportionately large segment of the total burden of disease associated with allergy. Excerpts are available HERE.
Another recent review article looks at the connection between metal hypersensitivity and implant failure. You can check the full article here: The contribution of metal allergy to the failure of metal alloy implants, with special reference to titanium: Current knowledge and controversies. A brief excerpt focused on several case reports of clinical reactions to implants is available HERE.
- List item:
- List title:
Increased reactivity to metals has been found in the following diseases:, List text:
• Multiple Sclerosis (Prochazkova 2003, 2006, Stejskal 2006)
• Chronic Fatigue Syndrome (Stejskal 1994, 1999)
• Rheumatoid Arthritis (Prochazkova 2003, Stejskal 2006)
• Fibromyalgia (Öckert 2006, Stejskal 2013)
• Amyotrophic Lateral Sclerosis (Pleva 2000)
• Cardiovascular disease (Manousek 2016)
• Lupus Erythematosis (Prochazkova 2003)
• Oral Lichen Planus (Stejskal 1996)
• Oral burning and itching (Stejskal 2006)
• Skin diseases such as eczema or psoriasis (Prochazkova 2003, Venclikova 2003, Kohdera, Ionescu)
• Sjögren’s syndrome (Prochazkova 2003)
• Alopecia areata and atopic alopecia (Nakayama and Chen 2018)
• Autoimmune thyroiditis (Sterzl 1999, Prochazkova 2003, 2010, Hybenova 2010)
, List image:
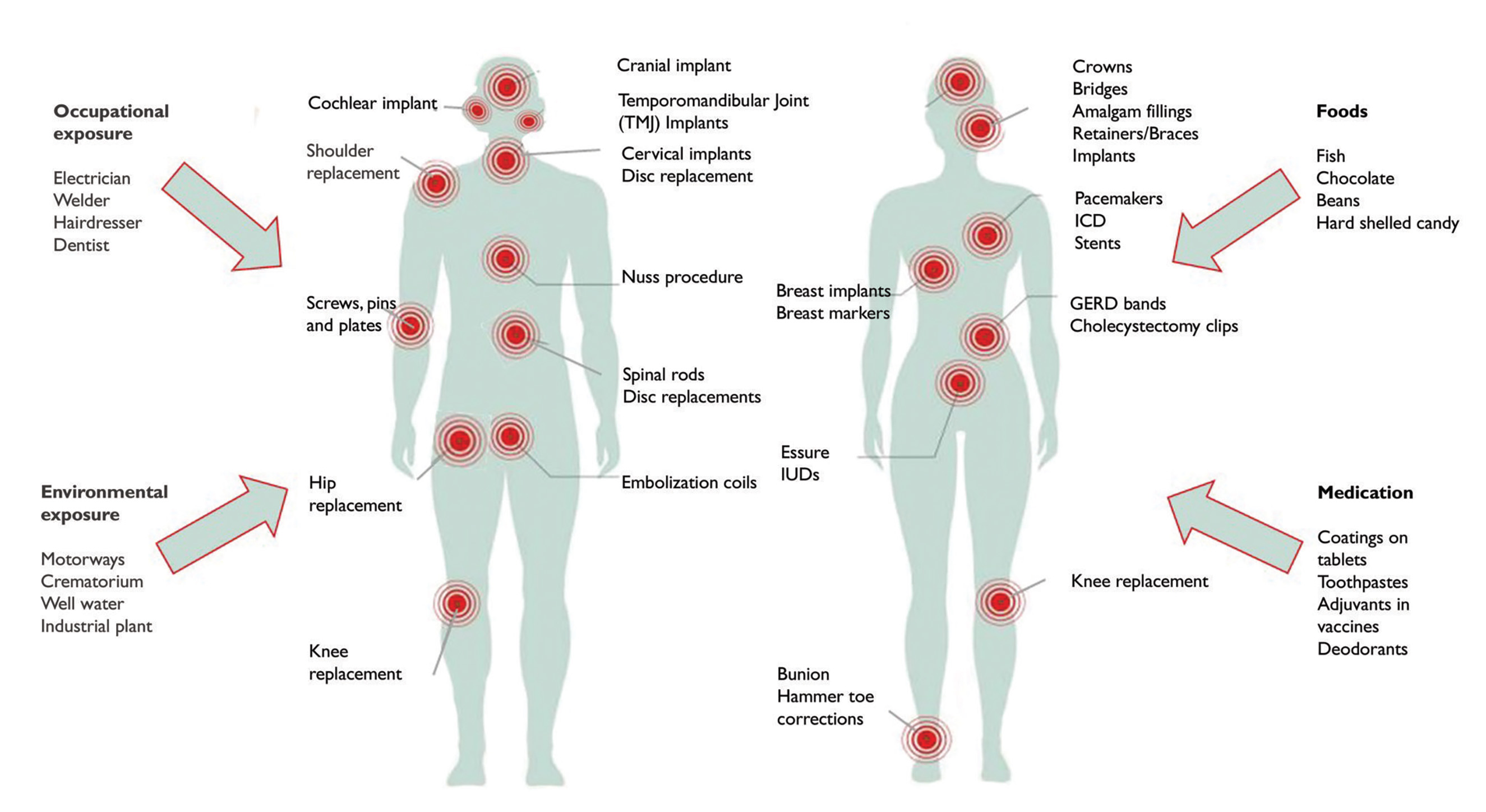
The prevalence of metal hypersensitivity in patients with implants is significantly higher than in the general population, with an even higher rate among patients with failed or failing implanted devices. (Hallab et al. Metal sensitivity in patients with orthopedic implants. The Journal of Bone and Joint Surgery 2001;83:428)
We are conducting a study to see if metals may be implicated in the development of scoliosis. Read more about the research HERE. - List title:
Treatment of diseases where metal allergy has played a part, List text:
As with any allergy, exposure to the offending allergen should be minimized or, if possible, avoided altogether.
, List image:
Metals can be found in food and also in medication, such as nickel and titanium dioxide, so in this case, patients might consider diets low in nickel. If a patient is allergic to a metal found in dental fillings or dental implants, it is important to consult a dentist who is experienced in the field of metal-free dentistry. The importance of being protected during the removal of, for example, amalgam fillings, cannot be overstated. Every dentist will have their own protocols, for instance, the SMART protocol from the International Academy of Oral Medicine and Toxicology (IAOMT). For many patients, avoiding metals will be enough for them to feel a significant health improvement.
- List title:
Increased reactivity to metals has been found in the following diseases:, List text: